If you have large, bulging varicose veins, endovenous laser treatment (EVLT) is an effective minimally invasive procedure that uses targeted laser energy to heat a vein from the inside, causing it to collapse quickly and eventually disappear.
About the Procedure
If your doctor thinks you're a candidate for EVLT, you'll first be given a venous reflux exam, a painless duplex ultrasound test to see how well or poorly the valves in your vein(s) are performing.
After you're given a local anesthetic, a very small hole is pricked in the skin (so small that stitches aren't needed), and a catheter is inserted into the vein. Through that catheter, a very thin fiberoptic laser probe is inserted. Your doctor will likely use ultrasound imaging to guide the placement of the catheter.
Once activated, the heat generated by the laser causes the walls of the vein to collapse and eventually disappear. With the use of local anesthetic, the procedure tends not to be painful — the worst discomfort is usually from the multiple injections of local anesthetic.
What Is EVLT Used For?
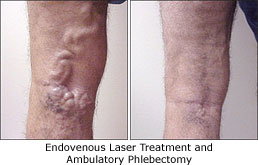 Although it can be performed for cosmetic reasons, EVLT is typically used when there are symptoms like swelling, ulcers, aches, etc. — particularly when a saphenous vein (one of several larger, deeper veins in the legs) isn't functioning properly. If the vein is twisted, however, EVLT is not an option. The saphenous vein that is eliminated is not functioning properly in the first place, so the procedure doesn't have a deleterious effect. It should relieve the symptoms, and the blood will find its way back to the heart through other, properly functioning veins.
Although it can be performed for cosmetic reasons, EVLT is typically used when there are symptoms like swelling, ulcers, aches, etc. — particularly when a saphenous vein (one of several larger, deeper veins in the legs) isn't functioning properly. If the vein is twisted, however, EVLT is not an option. The saphenous vein that is eliminated is not functioning properly in the first place, so the procedure doesn't have a deleterious effect. It should relieve the symptoms, and the blood will find its way back to the heart through other, properly functioning veins.
EVLT Recovery, Risks, Side Effects and Complications
EVLT is very effective, with excellent results after a single treatment — better than sclerotherapy, and about the same as endovenous radiofrequency ablation.
The procedure usually takes an hour or so and is done on an outpatient basis or in the doctor's office. You can resume normal activity right away, except for flying or taking long car trips. You'll also need to wear a compression bandage for at least a few days. No extra bed rest — you should remain active.
EVLT doesn't leave visible scars. Side effects are typically minimal, but can include tenderness and bruising. The compression bandage helps with that. The vein can also get inflamed (thrombophlebitis), which can be painful, but over-the-counter anti-inflammatory pain medications usually help.
Less common complications include heat damage to nearby nerves, which can occasionally cause localized numbness, though it should go away over time. Infection is a possibility with any surgical procedure.
With EVLT there have been rare cases of deep-vein thrombosis (DVT), a condition where a clot forms in a vein. If that clot breaks loose, it can cause a potentially life-threatening pulmonary embolism. The Society for Vascular Surgery and the American Venous Forum, in their clinical practice guidelines, suggest doctors perform another duplex ultrasound 1 or 2 days after the EVLA procedure to be sure there are no clots.
Does Insurance Cover EVLT Treatment?
If EVLT is performed out of medical necessity, the procedure is usually covered by most insurance policies. Of course it's always a good idea to check with your insurer, because some insurance companies have very specific criteria for what constitutes medical necessity. Many insurers require you to try conservative therapy like compression stockings before authorizing EVLT or other procedures.
Alternatives to EVLT
EVLA is one of four primary treatment options currently in use in the United States to strip out larger veins. The other three are:
- Endovenous radiofrequency ablation, which is very similar to EVLT, except that the heat in the vein is generated through radiofrequency energy instead of light
- Ultrasound-guided sclerotherapy, in which an irritant (often a foam) is injected into the vein, damaging it and causing it to collapse
- Traditional open surgery to strip out the vein (no longer widely used in standard cases in the U.S.)
Reviewed February 13, 2017


