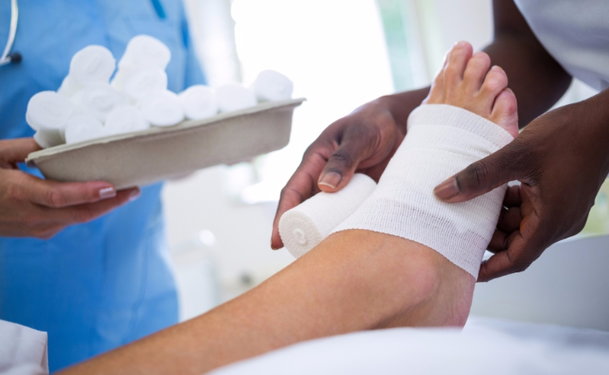
Faster healing is the goal of all wound management programs, including those for venous ulcers, also known as stasis ulcers. Compression therapy is the main treatment for venous ulcers. However, your doctor will work with you to choose the best wound management program for your needs.
Managing venous ulcers
Venous ulcers are a very challenging condition to live with because they can have such a significant impact on your quality of life. The condition is difficult to treat and will often return. Open ulcers may remain unhealed for weeks to many years. Venous ulcers can lead to significant medical complications, so proper treatment is very important.
Several factors can improve venous ulcer healing, such as making sure the wound is clean and free of bacteria, that you are eating healthy to support wound healing, and that there is good blood flow to the area. Quitting smoking and maintaining a healthy weight will also reduce your risk of developing a venous ulcer and speed wound healing.
The goals of wound care management are to reduce swelling, improve healing of the ulcer and keep the ulcer from coming back. Treatments include:
- Compression therapy. This is a common treatment for venous ulcers and can decrease the chance that a healed ulcer will return. Compression therapy reduces swelling and encourages healthy blood circulation.
- Leg elevation. This is often used alongside compression therapy to reduce swelling. The legs are elevated for around 30 minutes three or four times a day.
- Vacuum-assisted closure. This method reduces pressure over a wound (vacuum) through a special dressing. This draws the edges of the wound together and sucks out moisture and bacteria.
- Aspirin. When used alongside compression therapy, aspirin may improve healing by preventing the blood from clotting.
- Antibiotics. These may be useful when your doctor suspects that the skin in or near the ulcer is infected.
- Debridement. This involves removing damaged tissue from the wound.
- Human skin grafting. Healthy skin is taken from one area of a person’s body and grafted onto the wound in order to speed up healing.
- Surgery. This may be used to treat severe venous ulcers by repairing weak valves or removing blood clots. Surgery may also help keep the venous ulcer from returning.
Types of compression therapy
Compression therapy can speed up wound healing, as well as reduce swelling and pain. This type of therapy may be needed for months until the wound is fully healed. Ongoing use of compression therapy can also reduce the risk that an ulcer will come back.
Several types of compression therapy are available, including:
- Inelastic. This increases pressure on the wound while a person is walking or contracting the leg muscles, but not while at rest. The most common type of inelastic compression therapy is a moist bandage which hardens after drying. Because it is stiff, the dry bandage will not change when the size of the leg changes, which can be uncomfortable.
- Elastic. This type of compression therapy increases pressure on the wound both while moving and at rest. Both compression stockings and bandages can be used for this. Unlike inelastic compression therapy, this type can be removed at night, washed and easily replaced.
- Intermittent pneumatic compression. With this therapy, a pump is used inflate and deflate sleeves on the foot or leg. As the sleeve inflates, the pressure increases. Because the equipment is expensive and bulky, it is more commonly used for patients who are bedridden.
Signs and causes of venous ulcers
Venous ulcers are non-healing or slow-healing wounds that form as a result of blood pooling in the legs and feet. This happens when the walls or valves in the veins of the lower extremities don’t work effectively. This is called venous insufficiency.
Venous ulcers are more common in women and older people. Several factors increase your risk of developing venous ulcers, including:
- Long periods of immobility, such as bed rest
- Older age
- Obesity
- Leg injuries
- Deep vein thrombosis, or a blood clot, in one or more of the deep veins
- Family history of chronic venous insufficiency
- Phlebitis, or inflammation of a vein
Even before venous ulcers form, patients may experience venous stasis, or pooling of blood in the legs and feet. Symptoms include:
- Dull ache or pain in the legs or feet
- Swelling that goes away when you elevate the legs
- Changes to the skin that resembles eczema
- Varicose veins
Venous ulcers will often appear over bony parts of the legs and feet, such as the inner ankle. If an ulcer often shows up in the same area, this may be a sign of a venous ulcer. A venous ulcer looks irregular and shallow. There may also be swelling, inflammation, discoloration or thickening of the skin in the area near the ulcer.
Related wound types
Venous ulcers are the most common type of ulceration on the legs and feet. Ulcers can also be caused by lack of blood flow in the arteries, diabetic neuropathy, rheumatoid arthritis or skin problems.
Updated on Aug. 10, 2017