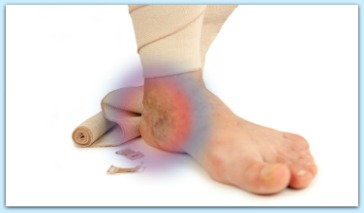
Venous ulcers, also known as venous stasis ulcers are open sores in the skin that occur where the valves in the veins don’t work properly and there is ongoing high pressure in the veins.
This causes blood to collect and pool in the vein, leading to swelling in the lower leg. Eventually non-healing or slow-healing wounds may form, often on the inside of the leg or just above the ankle. Venous ulcers can be painful and are a difficult condition that can severely affect your quality of life, but several therapies are available to relieve your symptoms and speed healing.
Wound care for venous ulcers
Wound care is an important part of treatment for venous ulcers. The goal of wound care management is to encourage the ulcers to heal more quickly. This includes:
- Compression stockings or bandages. These provide pressure on the legs to push blood toward the heart. The stockings or bandages also reduce swelling and pain in the lower legs.
- Unna boot. A moist gauze bandage is wrapped around the lower leg. It hardens to form a snug boot that helps push blood out of the legs. This provides less movement than compression stockings.
- Oral or topical antibiotics. If the wound becomes infected (such as cellulitis), your doctor may give you antibiotics to clear up the infection.
- Aspirin or other anti-clotting medications. Your doctor may ask you to take one of these medications to help your ulcer heal more quickly. This treatment is still being studied by researchers to see if it is effective.
Surgical treatments for venous ulcers
Several surgical procedures are available to treat the wound directly or address an underlying problem, including:
- Debridement. Infected tissue is removed surgically, along with foreign debris and material left behind from previous dressings. This is often done if the ulcer shows signs of infection.
- Sclerotherapy or endovenous ablation. The affected vein is destroyed using a chemical injected into it (sclerotherapy) or heat produced by laser or radio wave energy (endovenous ablation).
- Phlebectomy. A small hook is used to remove the veins that are affecting the ulcer in sections through several small cuts (incisions) in the skin.
- Ligation and stripping. The affected vein is tied off and then surgically removed.
- Valve repair. Sutures are used to help a valve stay shut. A healthy valve may also be transplanted from another vein into the affected vein.
Causes of venous ulcers
When the walls or valves of the veins are weak or don’t work properly, blood in the veins can flow backwards and pool in your legs. Valve problems can result from vein disorders such as chronic venous insufficiency (CVI) or deep vein thrombosis (DVT).
Veins have valves inside them that normally keep blood from flowing backwards. The valves are especially important in the legs, because gravity pulls the blood down toward the feet, making it more difficult for it to flow toward the heart.
CVI is an ongoing condition in which the walls or the valves of the veins don’t work properly. DVT is when blood clots form in deep veins, which can damage the valves. A small number of people are also born without valves in their veins, which can also cause blood to flow backwards in the veins.
Pooling of the blood (stasis) increases the pressure in the legs, which prevents oxygen and nutrients from getting to the tissue. This causes damage to the nearby tissue and forms a wound. Damage to the vein walls may also cause the release of compounds that damage the tissue even more.
Signs and symptoms of venous ulcers
Symptoms may show up even before an ulcer forms, such as:
- Swelling, heaviness or cramping in the legs
- Hardening or thickening of the skin (lipodermatosclerosis)
- Dark red, purple or brown discoloration (hyperpigmentation)
Signs and symptoms of venous ulcers include:
- Sore on the inside of the leg or just above the ankle. The base of the wound is red and is sometimes covered by yellow tissue. The edges of the ulcer may be unevenly shaped.
- Skin around the wound is shiny, warm or hot, tight and discolored.
- Pain in the leg.
- If the wound becomes infected, it may smell bad and pus may drain from the sore.
Risk factors for venous ulcers
The following will increase your risk of developing venous ulcers:
- Varicose veins, which are swollen, twisted veins visible just beneath the surface of the skin
- If you’ve had blood clots in the leg before
- Family history of venous insufficiency or deep vein thrombosis
- Older age
- Being tall
- Being female
- Obesity
- Pregnancy
- Sitting or standing for long periods
- Smoking, which can increase your risk of blood clots
- Damage to the veins of the legs, such as from an injury or surgery