 Vein decided to interview Dr. Kathleen Gibson because of her unusual standing as a private practitioner who is significantly involved in vascular disease research and clinical trials. She is a partner with Lake Washington Vascular Surgeons PLLC, with four locations in the Seattle, Washington area. She has been a principal investigator for more than 20 clinical trials. Dr. Gibson was the first female vascular surgery fellow at the University of Washington and the last fellow to work in the laboratory of the late Dr. Eugene Strandness, father of the duplex ultrasound, before he died in 2001.
Vein decided to interview Dr. Kathleen Gibson because of her unusual standing as a private practitioner who is significantly involved in vascular disease research and clinical trials. She is a partner with Lake Washington Vascular Surgeons PLLC, with four locations in the Seattle, Washington area. She has been a principal investigator for more than 20 clinical trials. Dr. Gibson was the first female vascular surgery fellow at the University of Washington and the last fellow to work in the laboratory of the late Dr. Eugene Strandness, father of the duplex ultrasound, before he died in 2001.
I had the pleasure of interviewing Dr. Gibson in August right after she returned from a life-changing trip as a volunteer physician with Amigos de Salud, a U.S.-based, nonprofit medical organization founded by the Morrison Clinic. She discusses that trip in this interview, as well as some of the challenges and unique aspects of her career thus far. As a vascular surgeon and co-medical director of one of Washington state's busiest diagnostic vascular laboratories, Dr. Gibson specializes in minimally invasive vascular techniques including aortic stent grafts, peripheral angioplasty and stents (venous and arterial), endothermal heat ablation for superficial venous insufficiency and sclerotherapy.
Dr. Gibson, you were recently out of the office for a 10-day medical volunteer trip to Matagalpa, Nicaragua. What would you like to share with your peers about that experience?
The trip was fantastic and life changing. In Nicaragua, there is no need for insurance preauthorization and no electronic medical record, so you get to meet patients, figure out what's wrong with them and then treat them very quickly. It's kind of like what medicine must have been like a long time ago. Patients are extremely grateful and they trust you. Their disease is often very advanced, and they're happy for whatever you can do for them. The group I went down with was led by Dr. Nick Morrison, a founder of Amigos de Salud. It's a nonprofit that annually brings medical volunteers together who travel to developing countries at their own expense to examine and treat patients through diagnostic and interventional procedures. This is their 25th year of going to either Ecuador or Nicaragua.
We were in a town called Matagalpa, one of the largest cities in Nicaragua, located in the mountains with a climate not as hot and humid as lower elevations. We went to a clinic built by the Fara Foundation, which was established by the owners of Fara Coffee, an American/Nicaraguan coffee company. The patients we saw were all vein patients, or patients with venous wounds.
There were eight doctors there, including myself and Dr. Morrison from the United States, a doctor from Australia, a doctor from Argentina and four Italian doctors. My team consisted of Merrie Leiderman, RVT and Jean Klein, RN, from Lake Washington Vascular. I also brought my teenage daughter along and Jean brought her teenage son. My staff gave up a week of vacation time to go to Nicaragua. It was a very personally fulfilling experience.
It was very rewarding to interact with colleagues from other countries. We would all have dinner and lunch together, and discuss the differences in how vein care is being delivered in our respective countries. We would walk to Fara clinic every day in our scrubs. The whole group treated about 650 patients in six days. We worked long hours and had to be very efficient.
An eye-opening experience for me involved treating a woman who had 10 children. She was a little nervous, so to calm her, I talked about my family, and asked about hers. I have three dogs, and I asked her, "Do you have animals?" This woman responded that she had a pig. I thought that was kind of unusual--to have just one pig, so I asked her why. She explained, "If one of my children gets sick, we can sell the pig for medicine."
So the pig was her insurance! We have Aetna, Blue Cross and other insurance plans--and that Nicaraguan woman has a pig. Their culture is so very different than what we experience here in the United States.
Medtronic and Summit Imaging generously provided us with equipment for the trip--a radio frequency generator and an ultrasound machine. We brought a laptop ultrasound with us, and there was already a laser machine there donated by Dr. Morrison a number of years ago. Other volunteers brought their own equipment.
It's definitely challenging doing research without the support of an academic institution. You have to be organized and have plenty of help but it's entirely possible to conduct research while in private practice.
Are you planning to volunteer again next year?
Yes, I would love to go again in the future. I know there are a lot of other doctors that want to go down to Nicaragua with Dr. Morrison, and everyone that wants to go, doesn't necessarily get to go but I would hope that we did a good enough job that they would want us to come back with the group again someday. Dr. Gibson, you specialize in minimally invasive vascular techniques. How did Dr. Donald Eugene Strandness and his pioneering "Revolution in Noninvasive Vascular Diagnosis" affect your career?
Dr. Gibson, you specialize in minimally invasive vascular techniques. How did Dr. Donald Eugene Strandness and his pioneering "Revolution in Noninvasive Vascular Diagnosis" affect your career?
Yes, it's well known that Dr. Strandness developed the duplex ultrasound with a partner here in Seattle. We still use it for imaging. He was Chief of Vascular Surgery at the University of Washington for many years, and very involved in clinical research. I was the last fellow to work in his lab before he died in 2001. He had a profound influence on me and was kind of like a second father. A lot of my career values and goals come from his mentorship.
I was training at the University of Washington in general surgery and I didn't know at the time what specialty I wanted to pursue, but as I went through my residency, I discovered I liked vascular surgery. That's where I met Dr. Strandness. The vascular surgeons were very kind and I felt an affinity toward them. At that time, they'd never had a female vascular surgery fellow at the University of Washington and Dr. Strandness wanted to rectify that, so he encouraged me to apply. Back then, you were required to conduct research the first year of your fellowship. I knew I wasn't interested in doing basic science--I was more interested in duplex ultrasound and clinical research, so I naturally gravitated toward his lab.
When I was finishing the fellowship and decided I wanted to go into private practice, Dr. Strandness said, "You're making a big mistake. You should be in academics, because you're a good teacher and you like doing research. I give you five years, and you'll be back in academics." I did not go back into academics, but I did become involved in clinical research about five years after finishing my fellowship.
Yet you have done major clinical research while never being at an academic institution. That must be challenging. Tell us about your research efforts.
It's definitely challenging doing research without the support of an academic institution. You have to be organized and have plenty of help but it's entirely possible to conduct research while in private practice. I have four partners and they are often sub-investigators, or principal investigators themselves. We have two clinical research coordinators on staff and we also have a research assistant. We don't do basic science research. We do clinical research including drug and device trials.
Although the technology is pretty standard at this point, the changes we've seen in venous disease over the last 10 to 15 years are enormous. Some of the revolutionary changes in arterial surgery were already happening when I was in training, but I've had 14 years in practice now and what used to be done in hospitals is now done in the office. We're learning more and more about areas such as deep venous reconstruction and new anticoagulants for treating thrombotic disease.
One area I'm particularly interested in is Pelvic Congestion Syndrome, including the treatment of women who develop vulvar varicose veins after pregnancy. Women may be embarrassed to bring up this issue with their primary care doctor or OB/GYN, which would probably be the first person they would talk to. There isn't a lot of knowledge about this condition, which in many respects is the female equivalent of a man's varicocele. Referring doctors often don't know where to send these patients. The recognition of the problem becomes delayed, so the women I see in my practice often have been having problems for years before they see me. Controversy exists about how these patients should be imaged, diagnosed and treated. It's an area in which I hope more papers and research will focus, because we need more data.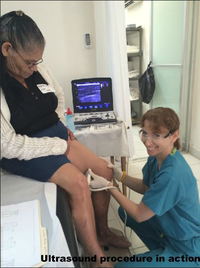 Do you currently mentor other vein specialists? How do you go about highlighting the opportunities and challenges in vascular surgery for new fellows?
Do you currently mentor other vein specialists? How do you go about highlighting the opportunities and challenges in vascular surgery for new fellows?
Since I'm in private practice, I don't have medical students or fellows working directly with me, but I am involved in education within societies--particularly the American Venous Forum's Fellows Course. I was the chair last year and have been involved with teaching for a number of years, so I've been able to get to know some of the upcoming vascular surgeons and interventional radiologists and other young doctors interested in phlebology. Some of them have come to our clinic for short periods of time for learning purposes.
The Fellows Course was founded because there was a huge gap in educating fellows about venous disease. They were receiving arterial education but not a sufficient venous education. So unless that changes in fellowship programs, there will always be a place for AVF's Fellows Course. Another value of AVF Fellows Course is networking and mentorship. It's good for fellows to meet other peers interested in veins throughout the country.
Finally, we also teach ethical behavior in that course. One of the issues we've had with superficial venous disease in particular was that when new techniques first came out, reimbursement was very good, so a lot of people flocked to treating veins but were not necessarily focused on patient outcomes or doing the right thing for their patients. The AVF Fellows Course helps to ground the Fellows and teaches them to better listen to patients.
Besides the American Venous Forum, what other professional organizations do you devote time to? What accomplishments for those organizations are you particularly focused on?
I'm on the boards of the American College of Phlebology and the American Board of Venous and Lymphatic Medicine. Next year my fellow board member Carl Black and I will be convening the ACP’s annual congress.
I am a member of the European Venous Forum and I love going to that meeting when I can take time to attend. It's interesting and fun to learn from our European colleagues because they do things differently. They have the same kind of patients, same kind of problems but different approaches to treatment that end up with the same results. It makes you realize there are many correct approaches to the same problem. The reasons to pick one or the other might be based on what your peers are doing or on culture. I believe it's good to learn from other people, so you don't get stuck in the mindset of "my way is the only way."
For example, vein stripping is still the number one procedure in the world for treating the great saphenous vein, while in the United States it has fallen out of favor. There are places where it's still being done, however. That procedure itself has evolved from the time I was in training in the 1990s; it's still being done but less invasively.
What is your next challenge regarding venous disease?
The next challenge for phlebology in general revolves around the fact that there are exciting new technologies that we can use but constraints on reimbursement from payors. I think that payors are reluctant to cover some of these new technologies, especially when they are not as cost effective as those currently used. One of the reasons I'm involved in research is because I'm intellectually curious and I want to try the new technologies. But we're inhibited by economics.
Some areas of challenge include deep venous procedures and patients who need iliac vein reconstruction. Who needs to be treated and who should be treated conservatively? As some of these new techniques are available, doctors may have the impulse to treat more and more patients and push the envelope. Some of those patients may not need these treatments. If there is a rapid increase in the number of procedures done, it will catch the attention of both governmental and private payors who may then determine that doctors are over-utilizing the treatment. We need to be very thoughtful about who needs treatment and who does not.
Having varicose veins can be a quality of life issue; the disease can progress and cause worse problems. If you look at the savings to society of keeping somebody from being disabled, and of helping them have healthier legs, you realize the treatments truly are cost effective. Many patients are young and otherwise healthy, and by improving their symptoms, you can give them years of improved quality of life
It's a matter of not only educating the public but also educating the patients themselves. There are patients who will see a primary care physician and are told, "varicose veins are not a medical problem," or "varicose veins that are treated will just come back." To me, that's not a good reason to avoid treating the problem. It's kind of like saying, "my yard is overgrown with weeds, so I'm never going to weed it."
What is the most fulfilling aspect of your practice?
It's definitely not the electronic medical record! (laughs) Patient care is what most fulfills me most. Nothing is more gratifying than having a skill that you've worked hard to master that you can use to help other people. What fulfills me most is not writing a paper, not giving a talk but doing what's best for my patients. And I have to say, vein patients are among the most grateful.


