 We both said “I do.”
We both said “I do.”
Three years ago we decided to add a certified nurse practitioner to our very busy practice. It was, and still is, one of the best decisions we have made.
Mid-Level Practitioners
Let’s start with proper and accepted definitions before we dive into how you can incorporate additional medical professionals into a busy vein practice.
The term "mid-level practitioner" is used by the United States Department of Justice Drug Enforcement Administration (DEA) to identify a group of health care individuals for the purpose of monitoring controlled substances.
According to the DEA Office of Diversion Control, "Pursuant to Title 21, Code of Federal Regulations, Section 1300.01(b28), the term mid-level practitioner means an individual practitioner, other than a physician, dentist, veterinarian, or podiatrist, who is licensed, registered, or otherwise permitted by the United States or the jurisdiction in which he/she practices, to dispense a controlled substance in the course of professional practice.
Examples of mid-level practitioners include, but are not limited to, health care providers such as nurse practitioners, nurse midwives, nurse anesthetists, clinical nurse specialists and physician assistants who are authorized to dispense controlled substances by the state in which they practice."
Medicare uses the term "non-physician practitioner" to describe advanced practice nurses (APN) and physician assistants (PA).
Defining team member roles in your vein practice
 Prior to hiring anyone into a busy vein practice, it is always recommended to define a role for your new found partner in venous medicine. Kendra Maag, RN, MSN, FNP-C saw an opportunity to work collaboratively in a growing field with room to grow the practice. “Our office is able to see more patients and do more advocacy work in the community in early recognition of venous disease,” she said.
Prior to hiring anyone into a busy vein practice, it is always recommended to define a role for your new found partner in venous medicine. Kendra Maag, RN, MSN, FNP-C saw an opportunity to work collaboratively in a growing field with room to grow the practice. “Our office is able to see more patients and do more advocacy work in the community in early recognition of venous disease,” she said.
Kendra’s initial role of seeing patients post-procedure has grown into assessing new patients and even come up with plans for long-term success in venous disease. She has also added several skill sets to her toolbox to include sclerotherapy and other cosmetic treatments.
She is also included as a staff member of the IAC accredited Vascular and Vein Center Laboratory. She spent a greater part of several months observing and training with me, and then quickly began evaluating patients. She then gained the other skill sets in the last year.
I made sure I introduced Kendra to the patients we would see together and decide their course of care as a duo. That allowed patients to know that they can trust her as well. We also spent some marketing dollars introducing her to the community via commercials, videos and social media outlets as well.
 “I feel I have added value to the practice and to the patient,” Kendra said. She has answered patient questions and referral questions many times, and she feels confident in her medical decisions with the comfort of having her physician collaborator at her side. “We are in constant communication and send notes back and forth within the EMR to make sure both of us are aware of outstanding concerns, questions, blood work, diagnostic tests, etc.”
“I feel I have added value to the practice and to the patient,” Kendra said. She has answered patient questions and referral questions many times, and she feels confident in her medical decisions with the comfort of having her physician collaborator at her side. “We are in constant communication and send notes back and forth within the EMR to make sure both of us are aware of outstanding concerns, questions, blood work, diagnostic tests, etc.”
In addition to good communication, it is imperative to know the rules and laws of the state that you practice in. Kendra and I have a collaboration agreement that is renewed yearly. Both the nursing and state medical board requires this type of agreement. Along with state board requirements, we have additional protocols to fulfill our IAC Vascular and Vein Center accreditation.
The hiring decision requires you to carefully consider several factors. You need to research state regulations and reimbursement rules.
The prescribing authority for medical professionals varies across the U.S., with some states allowing some to write prescriptions for all medications (including controlled substances) while others require a physician’s signature on prescriptions.
You must also consider that not all states allow all team members to order tests or to bill independently for their services. Lastly, some states require that a physician be onsite with a certified nurse practitioner or PA at all times, while other states allow that the physician be available by phone.
These requirements also differ between physician assistants and nurse practitioners, and state regulations may influence which specialty a practice decides to hire.
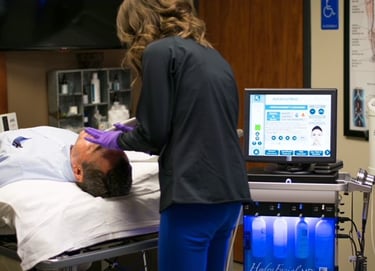 Empower your team members
Empower your team members
As the role of the physician is ever-changing and becoming more demanding, the additional medical professionals become key players in the success of quality patient care—and they love it. Empowering your team members to be integral in treating venous patients allows them to improve the processes within your practice.
There is still a lot of oversight and review of charts, images, reports, plans and more. However, including them in meetings, protocol development and quality improvement measures allows them to see how their care directly impacts patients and your practice’s success.
In order to empower others, the physician has to “let it go.” It is important to see what role you have and be able to delegate some of your duties to your partner. For example, Kendra sees most of the one-week follow-ups in our practice who have had a non-cosmetic venous procedure.
I spend time on Sundays calling all the patients from the week to make sure they are following their post-procedure care instructions we give them, and let them know they will either see myself or Kendra at their one-week follow-up. I also let them know that if they would like me to see them for any reason, at any time, to just ask.
Kendra and our registered technologists are empowered to share information with the patient, and it is liberating to allow them to take the lead on patient engagement and relationship building.
We do this because our team shares the same mission and vision. Giving authority to those not vested in your practice is pointless and will prove to be detrimental to the success and care of your patients.
Payment
According to the United States Bureau of Labor Statistics (BLS), the average income for PAs is $102,090, or about $49 an hour, though at the high-end of the salary range they may make more than $142,000 per year. Nurse practitioners earn an average salary of $104,610 per year, or roughly $50 an hour. The top 10 percent, typically those with considerable experience, earn an average of $140,930 per year.
Future growth
As of 2016, the BLS reported that there were 104,050 physician assistants practicing in the country. As of 2016, there were around 150,230 active nurse practitioners.
The BLS also reported that the number of jobs for PAs is expected to increase by roughly 28,700 between 2014 and 2024. That’s a 30 percent growth rate. The number of nurse practitioner jobs is expected to grow at a rate of 31 percent between 2014 and 2024, also much faster than average.
Return on investment
As more rules and regulations are placed on physicians regarding electronic medical records, registry participation and reporting, successful utilization of non-physician medical professionals is inevitable.
One sure way to optimize the use of a medical professional is to allow them to see the follow-ups on global patient encounters—and still bill at 85 percent of physician reimbursement. The one-week ultrasound can still be reviewed and signed by the physician.
However, the clinical visit is not billable as it falls in the 90-day global visit. Try to keep the same schedule to three-month and one-year follow-ups. This frees up the clinicians’ time to focus on other revenue generating tasks such as venous procedures and cash-based cosmetic procedures.
For example, in our practice, we have a set schedule that allows me to see cosmetic laser patients daily, along with a daily average of three to four venous procedures. This doesn’t include the schedule for two other ultrasound technicians, a licensed cosmetic therapist, a registered nurse and a certified lymphedema therapist in our practice.
Though our entire team is vital to the practice, Kendra and I can easily monitor, evaluate and care for many more patients a day together then I could separately.
Aside from generating an ROI by adding other medical professionals, the most important aspect is the creation of the team atmosphere; the helm of the practice is still the physician. This allows you to participate in the most critical aspects of patient care—ultrasound readings, plan/treatment review, etc.
This creation of a “work family” grows the practice as a whole, and each individual as a person. Assigning roles, empowering each member of the family within state and federal rules, and paying them a proper salary will prove to be successful for any practice.
So put a ring on it.


