 As wound care providers, we hold people’s lives in our hands. The five-year mortality rate of a person with a neuropathic foot ulcer is 45%, compared to 11% for a patient with breast cancer and 35% for a patient with colon cancer. These figures are truly staggering. We can do better. We must do better.
As wound care providers, we hold people’s lives in our hands. The five-year mortality rate of a person with a neuropathic foot ulcer is 45%, compared to 11% for a patient with breast cancer and 35% for a patient with colon cancer. These figures are truly staggering. We can do better. We must do better.
We know often times the ulcer itself is a symptom of a more serious underlying condition, and it may very well be this underlying condition that is leading to the high mortality of these patients. However, make no mistake, the ulcer itself causes significant morbidity and mortality. Often times this morbidity and mortality is associated with our multiple, failed treatment attempts. Multiple debridements, hospitalizations, surgeries, and antibiotic use takes it toll and absolutely contributes to this very high mortality rate.
That speaks to the seriousness of the condition we are dealing with. Now consider the urgency that is required in treating a diabetic foot ulcer. Is a new, uninfected neuropathic ulcer an emergency? Yes, it is! The Sheehan data tells us if an ulcer is not 53% smaller after four weeks of conventional treatment, there is only a 9% chance that it will go on to heal in the next 12 weeks. Think about that. Read that sentence again. Challenge yourself with that ambitious goal. Keep track of these measurements and see if you are getting ulcers 53% smaller in the first four weeks of treatment. If you see these patients every two weeks, you only have two visits to get the ulcer to be about half the size. From the first visit, the clock is ticking. You must ask yourself at that very first visit: “How am I going to get this to be half the size in four weeks?”
Many times proper offloading is the most important component in accomplishing this goal. There are several things to consider when choosing our method of offloading: cost, availability, ability of the patient to use it and, most of all, effectiveness. We can look at some of the options available.
Crutch option for non-venous wounds
Crutches seem to be a good option. The problem is that effectively maintaining non-weight bearing status using crutches is totally unrealistic and not safe for many of our patients with diabetic foot ulcers. Many of these patients are obese, deconditioned, and compromised such that their attempt to keep weight off of a foot using crutches is not possible for them and also presents a fall risk.
Other options for non-venous wounds

Wedge shoes are another option. Forefoot wedge shoes are often used in an attempt to offload plantar forefoot ulcers. However, we have studies that show us no statistically significant difference in the pressure to the plantar forefoot in a forefoot wedge shoe versus in a regular sneaker.
If you just take the time to watch someone walk in one of these shoes, you see that it often functions like a seesaw, with the patient rocking forward onto their forefoot and the front of the wedge shoe “clicking” against the ground. The same data exists for the rear-foot wedge shoe, showing us no difference in pressure absorbed to the plantar heel in this wedge shoe versus a sneaker.

As wound specialists, we should have some expertise in gait analysis. If you watch someone walk in one of these rear foot wedge shoes, the heel is resting on a rigid plank, and it is clear that the rear foot is bearing the full force of heel strike just as it does in a regular shoe.

A knee scooter, or hands-free crutch, works well with young, fit athletes who need to be non-weight bearing after an injury or a surgery. However, these are not safe for most of our diabetic foot ulcer patients, and there are weight restrictions with many of these devices that most of our patients will not meet.Another option is the removable cast walker with the liner in the plantar foot that has removable Velcro shapes to try to create an aperture affect about the plantar ulcer.
We know that what often happens with these is when the patient returns two weeks after creating this cut-out, the hole is twice the size of what we started with and the patient is complaining that the Velcro shapes are all over their house!
So where does that leave us? After going through these options, we haven’t answered our question as to how we are going to effectively offload a limb-threatening diabetic plantar foot ulcer to allow its size to decrease by 53% in four weeks. The answer is with a total contact cast.
In the study done by Nabuurs-Franssen, 98 consecutive ulcer patients with polyneuropathy were treated with total contact casting. Of the non-ischemic ulcers—we know underlying vascular disease must first be addressed—90% without infection healed and 87% with infection healed. Furthermore, the average time to healing was just 34 days. The Sheehan data left us with a goal of decreasing the size of an ulcer by 53% in 28 days and in this study, the ulcers healed by total contact casting were closed in an average of 34 days.
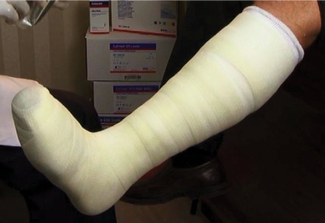
So why are so few practitioners using total contact casting? Of all the doctors in the country practicing wound care, only between 2% and 6% are using the total contact cast. This is a surprisingly low number given the power of this modality. Some say it’s too hard or they don’t know how. Application of a total contact cast is not a difficult skill to learn. With many of the newer kits that contain all the materials you need in one box, application can be done in less than 10 minutes after a bit of practice. Here is a video demonstrating application of a total contact cast.
Some practitioners who perceive the application of a total contact cast to be a burdensome, time-consuming venture, may say it’s not “worth it.” We have a responsibility to live up to our oath and save legs and save lives, and literature tells us using total contact casting can help us to accomplish those things. Of course it’s worth it!
Determining the value of non-venous treatments
If we must evaluate the “worth” of this treatment option from another angle, we can look at the practice management of total contact casting and find its importance is growing in this area as well. The way wound care providers are reimbursed is changing. We are seeing a change from a volume-based model to a value-based model.
By 2018, Medicare plans to link 50% to 90% of reimbursement to quality of care. They aim to accomplish this through alternative reimbursement models and quality measures. The concept of fee-for-service is shifting to “fee-for-results.” The days of billing CPT 97597 on the same patient every two weeks over and over and over for months on end with no wound progression and getting paid every time are ending.
Imagine yourself as the patient. You tear your ACL. Which would you prefer: the doctor who does your repair and gets paid the same no matter the quality of the repair, or the doctor who gets paid more if you have an earlier return to activity with a better long-term outcome?
A 62-year-old man with a diabetic foot ulcer would certainly prefer a situation where the doctor taking care of him is going to get paid more if she gets him healed more quickly with no complications and no surgery. Not only will the reimbursement model of the future take quality and results into account, but also the total cost of care provided will be considered in factoring the doctor’s reimbursement.
Developing a better reimbursement model for non-venous wound care
The Energy and Commerce Committee, together with the Secretary of Health and Human Services, says we need to “develop a payment model that will encourage better care in a more efficient manner.” Using total contact casting to treat pedal neuropathic pressure ulcers defines “better care in a more efficient manner.” Evidence-based medicine tells us that the total contact cast is better care.
Healing an ulcer in an average of 34 days, using casting material, is certainly more efficient than endless debridements, surgery, and trying four different types of topicals before ultimately failing and the patient having an amputation. If the cost of care provided is going to be considered in our reimbursement, then total contact casting will be an essential tool for excellent practice management.
That is a look at the future of reimbursement. In the present, the CPT code for application of a total contact cast is 29445. Look it up on the Medicare part B physician fee schedule in your area. In most areas of the country, it is assigned a non-facility fee of about $150. In a non-facility setting, the provider can also bill for the casting materials, which will add to the reimbursement.
It takes about 10 minutes to apply the newer total contact casts. You can do it more quickly with some practice, and even more quickly if you have some help in the office. For those who think they don’t have time to implement total contact casting into their practice, consider what is at stake: the value currently assigned to total contact casting and the value it will hold in the future. With that in mind, you may find that you can’t afford to NOT start using total contact casting.
Centers for Medicaid and Medicare Services' approach
CMS began to aggressively incentivize total contact casting in the outpatient hospital setting in 2015. Many wound care centers are considered an “outpatient hospital” place of service. In the Hospital Outpatient Prospective Payment System (HOPPS), total contact cast application is assigned an ambulatory payment classification (APC) of “0058.” In 2014, this was assigned a value of about $122, depending on where you are in the country. In 2015, this was increased by about $100, up to a national average of $223.
This was a dramatic change, which should increase utilization of this powerful modality. In addition to the facility itself billing, when a physician applies a total contact cast in a wound care center, the doctor can bill the 29445 CPT code and expect to collect the facility of about $115. This is an example of cost effective, well-reimbursed, excellent care. When a total contact cast is applied in this hospital outpatient setting, neither the doctor nor the center can bill the materials code, as the reimbursement to the center packages the application and the materials in that one APC.
Regardless of place of service, it is not appropriate to bill for ulcer debridement and total contact cast application for the same ulcer at the same time.
The total contact cast technique
Total contact casting can also have an impact on marketing your practice. Your reputation in your community among your patients, prospective patients, and referring doctors, is vital and becoming more important because it is becoming more and more readily available. Forty percent of Americans that use the Internet, use physician-ranking websites. Eighty percent of all new patients will use the Internet to Google their doctor before their first visit with that doctor.
How do you want to be known? What do you want patients and their family members posting about you? Patients who go to the same doctor every two weeks for six months and fill prescriptions for three different topical agents and are still not healed, are not going to be motivated to contribute excellent online reviews.
On the other hand, how likely is a perspective patient to make an appointment who reads this: “My wound was present for six months before I saw Dr. X, and she used a casting method that no one else had tried and my wound was gone in four weeks.” Now that’s practice management! Studies also show that potential referring doctors are even using these online physician-ranking sites to decide which specialist to refer to.
Potential referring doctors who read wonderful testimonials from your patients are more likely to refer their patients to you.
Conclusion
As wound care experts we need to do a better job. A five-year mortality rate of 45% is way too high. We can lower that. Keeping in mind that an ulcer that does not decrease in size by 53% in the first four weeks of treatment has only a 9% chance of healing in the next 12 weeks, we need to treat these ulcers with urgency and institute the offloading that is needed immediately. By using total contact casting when indicated, we can save legs, we can save lives, and keep our practices successful in today’s changing reimbursement climate.
Dr. Lehrman is on the APMA Coding Committee, is an expert panelist on Codingline, and is a Fellow of the American Academy of Podiatric Practice Management (AAPPM). He is on the Board of Directors of the ASPS and the APWCA. Follow him on Twitter.
References:
- “5 Tips on Moving Away from RVUs for Physician Compensation” Becker’s Hospital Review 4-30-13 Sabrina Rodak
- “The 4 ‘Hanging Chads’ of the Patient Protection and Affordable Care Act” Becker’s Hospital Review 5-20-13 Bob Herman
- “Physicians, Lawmakers Nearing Consensus on Doc Pay System,. But Cost Remains Issue” Bloomberg BNA 5-8-13
- Fleischli JG, Lavery LA, Vela SA, et al. “Comparison of strategies for reducing pressure at the site of neuropathic ulcers”. J Am Podiatr Assoc 1997;87(10):466–472.
- Diabetes Care. 2003 Sep;26(9):2595-7. „Activity patterns of patients with diabetic foot ulceration: patients with active ulceration may not adhere to a standard pressure off-loading regimen. Armstrong DG1, Lavery LA, Kimbrel HR, Nixon BP, Boulton AJ
- Wound Repair Regen. 2010 Mar-Apr;18(2):154-8. Epub 2010 Feb 16. “Why is it so hard to do the right thing in wound care?” Fife CE1, Carter MJ, Walker D
- Sheehan et. al. Diabetes Care. 2001; 25


