Although lipedema was first described by Drs. Edgar Allen and Edgar Hines in 1940 at the Mayo Clinic, many physicians remain unaware of this medical condition or its symptoms (Hines, 1940). Lipedema is a chronic, progressive medical disease that causes a disproportionate amount of swollen fat deposition in the arms and/or legs. As lipedema worsens, the affected limbs feel heavy and can be painful. The condition is associated with easy bruising, especially in the affected limbs. As a result of the lack of awareness, many patients are not diagnosed or properly treated, or are not treated until they have progressed to more advanced stages of the disease.
Although lipedema was first described by Drs. Edgar Allen and Edgar Hines in 1940 at the Mayo Clinic, many physicians remain unaware of this medical condition or its symptoms (Hines, 1940). Lipedema is a chronic, progressive medical disease that causes a disproportionate amount of swollen fat deposition in the arms and/or legs. As lipedema worsens, the affected limbs feel heavy and can be painful. The condition is associated with easy bruising, especially in the affected limbs. As a result of the lack of awareness, many patients are not diagnosed or properly treated, or are not treated until they have progressed to more advanced stages of the disease.
Cause of Lipedema and Pathogenesis
Though the exact cause and pathogenesis of lipedema is unknown, it is thought to be a genetic disorder with autosomal dominant inheritance and sex limitation (A.H. Child, 2010). This is because it occurs much more frequently in first-and second-degree relatives of affected individuals—reported rates of family clustering are from 16% to 64% of cases (L.E. Wold, 1949) (C.A. Harwood, 1996)—and usually occurs in women, although it can occur in men. Hormonal influences play a role in the development and progression of the disease and, in the majority of patients, the disease usually starts imperceptibly after puberty, but may also develop at other periods of hormonal change, such as pregnancy or menopause.
Grading of Lipedema
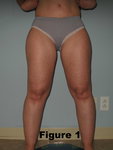
Stage I: In the first stage, the skin is smooth and the subcutaneous layer is thickened, soft, possibly with small nodules and even structure. The skin may be cool in certain areas as a result of functional vascular imbalance (see figure 1).
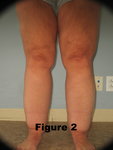
Stage II: Subcutaneous nodules and the skin’s surface becomes uneven (see figure 2).
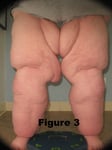
Stage III: Patients have huge amounts of tender subcutaneous tissue and bulging protrusions of fat, often at the inner side of the thighs or knees or gluteal area (see figure 3).
Signs, Symptoms and Progression of Lipedema
Individuals with lipedema have a marked discrepancy between the slim upper body and lower body, symmetrically enlarged with subcutaneous fat. This is often called the two-body condition, where a top half of the body may be a size 6 and the lower half of the body is a size 16. In the vast majority of women with lipedema, the thighs and hips are affected, and often the lower legs are affected as well. The upper arms are affected in about one-third of lipedema patients, with a smaller percentage having the forearms to the wrist involved (Krankheitsspektrum, 1997).
Early on, most patients with lipedema experience either no symptoms or mild symptoms. Often in the early stage, the fat accumulation may appear similar to the much more common cellulite fat. As the condition progresses, however, the fat hyperplasia becomes lumpier and more disproportionate than regular cellulite fat to a trained observer.
Women with lipedema report a spontaneous feeling of pressure or swelling and a hypersensitivity to touch and pressure in the thighs and lower legs. It is thought that there is inflammation in the subcutaneous fat, with an unregulated expression of inflammatory markers. Similar to vein disorders, the symptoms generally worsen as the day progresses, particularly after standing or sitting for long periods. Easy bruisability is reported, with minor bumps creating bruising. It is thought that the swelling is the result of a disturbance of the handling the extracellular fluid before it enters the lymphatic system (Streeten, 1973).
Lymphatic flow is usually preserved, and they usually have normal lymphoscintigrams, especially early on. Over time, though, the hyperplasia of fat in the subcutaneous tissue can begin to affect the channels of lymphatics, and they can develop a secondary lymphedema.
The fatty accumulation can affect mobility, and the disproportionate fat accumulation can become very distressing, especially if there is no recognition or understanding of its cause, which can lead to depression and social isolation. The secondary weight gain often occurs with patients who become distressed over this painful and possibly disfiguring condition.
These two factors can lead to calorie balance excess—eating more calories than expending through activity—which subsequently leads to a cycle of increasing obesity. Later in the course, lipedema patients may develop overt swelling with lipolymphedema, if they also become secondarily obese, which can interfere with lymphatic drainage.
Lipedema/Lymphedema Confusion
In Germany and the Netherlands, lipedema is well-known, and there are many textbooks and articles written about the condition. In the United States, even though it was originally described here, lipedema is not well-known, and articles and texts are few. This results in a confusion and lack of recognition. Obesity, which causes increased fat all over the body, including the stomach, is sometimes confused with lipedema—lipohypertrophy, or cellulite, also causes a disproportionate amount of fat accumulation in the legs, but does not cause pain or swelling.
Lymphedema is also often confused with lipedema. Lymphedema is asymmetric swelling of the limbs and often only one arm or leg is affected. Additionally, lymphedema causes swelling down to the feet and hands, whereas lipedema spares the hands and feet. Lymphedema is not painful or associated with easy bruising like lipedema. Chronic venous insufficiency can cause swelling and pain; however, it is not usually symmetric, has associated and characteristic skin changes, and usually has varicose veins.
Treatment of Lipedema
Conservative therapy with combined decongestive therapy (CDT) has a long track record of treating lipedema. The central component of CDT is manual lymphatic drainage (MLD), which is light massage therapy started centrally with a pump-and-scoop motion toward the heart. The manual lymph drainage is combined with compression wraps to complete the CDT. This conservative therapy can bring a reduction in circumference of approximately 10% and improves pain and symptoms of hypersensitivity to pressure. If the CDT is discontinued, the swelling and symptoms return. Compression stockings, which often need to be custom fitted, can be helpful in maintaining progress of combined decongestive therapy.
Surgical treatment has become much more common in the last 15 years and offers a greater chance of sustained improvement. Liposuction surgery of old was performed with general anesthesia, not tumescent anesthesia, and was associated with post-surgical complications and lymphatic vessel damage, and was not an effective lipedema treatment. However, modern tumescent liposuction performed with a wet tumescent technique is not associated with significant bleeding and does not damage superficial lymphatic vessels, according to macroscopic and anatomical studies (A. Frick, 1999) (J.N. Hoffmann, 2004).
The application of blunt micro cannulas measuring 2mm – 4mm allows surgeons to use a gentler technique and avoid damaging important structures, which results in a faster recovery and a significant net improvement of lipedema symptoms. I have modified the liposuction technique developed by Drs. Jeffery Klein and Stefan Rapprich (S. Rapprich) to include preoperative assessment and mapping of the proximal greater saphenous system to locate the lymphatics to minimize the chance of lymphatics injury.
The tumescent liposuction procedure not only improves physical appearance by returning some balance to the body’s proportion, it also can significantly reduce and eliminate the symptoms. Post-operatively combined decongestive therapy should be initiated or continued along with strict adherence to compression.
Long-term studies show that true tumescent liposuction can result in improvement of fat reduction, if performed properly by surgeons. It can reduce the circumference of the hips and lower extremities, balancing the disproportionality of the upper and lower parts of the body, and can improve or contribute to the relief of pain and pressure sensitivity. It can even reduce bruisability over an extended time period (S. Rapprich). However, the tendency for edema usually persists, and physical therapy and compression is often still necessary for patients, though to a lesser degree.
In conclusion, tumescent lipedema liposuction surgery is a great lipedema treatment and provides significant improvement in body shape, symptoms, and mobility. It also lessens the need for conservative treatment and significantly increases quality of life. Because of the level of expertise and understanding required to successfully perform tumescent liposuction surgery on these patients, they should seek treatment in centers where the surgeon and staff are specifically trained in lymphology and the needs of these unique patients. Thanks to Stanley Rockson, MD for assistance with the preparation of this article.
Works Cited
A. Frick, J. H. (1999). Liposuction Technique and Lymphatic Lesions in Lower Legs: anatomic Study to Reduce Risks. Plastic Reconstructive Surgery, 103, 1868-1873.
A.H. Child, K. G. (2010). Lipedema: An Inherited Condition. American Journal Med Genet, 152, 970-6.
C.A. Harwood, R. B. (1996). Lymphatic and Venous Function in Lipedema. BR J Dermatol.
Hines, A. E. (1940). Lipedema of the Legs: A Syndrome Characterized by Fat Legs and Orthostatic Edema.
Rochester, MN: Staff Meet Mayo Clinic.
J.N. Hoffmann, J. F. (2004). Tumescent and Dry Liposuctionof Lower Extremities: Differences in Lymph
Vessel Insury. Plastic Reconstruction Surgery, 113, 718-724.
Krankheitsspektrum, H. U. (1997). des Lipödems an einer Lymphologischen (Vol. 5). Germany: Fachklinik –
Erscheinungsformen, Mischbilder und Behandlungsmöglichkeiten, vasomed.
L.E. Wold, E. H. (1949). Lipedema of the Legs: A Syndrome Characterized by Fat Legs and Edema (Vol. 34). Ann
Intern Med.
S. Rapprich, A. D. (n.d.). Liposuction is an Effective Treatment for Lipedema Results of a Study with 25
Patients. JDDG (Journal of the German Society of Dermatology). doi:10.1111/j.1610-0387.2010.07504.x
Streeten, D. T. (1973). Studies of the pathogenesis of idiopathic oedema; the roles of postural changes in plasma
volume, plasma renin activity, aldosterone secretion rate and glomerular filtration rate on the retention of sodium
and water. In D. T. Streeten, Clinical Science and Molecular Medicine (pp. 347-373).