 Technological advances have resulted in our work tasks becoming more sedentary, which is in contrast to the needs of the human body. Musculoskeletal disorders associated with work tasks have increased over the years in many industries, including those among medical imaging professionals and health care providers. These injuries impact productivity, the quality of patient care and staffing levels.
Technological advances have resulted in our work tasks becoming more sedentary, which is in contrast to the needs of the human body. Musculoskeletal disorders associated with work tasks have increased over the years in many industries, including those among medical imaging professionals and health care providers. These injuries impact productivity, the quality of patient care and staffing levels.
The increased incidence of work-related musculoskeletal disorders (WRMSD) among these workers is due to several factors, including technological advances, less time for muscle recovery between work tasks, busier schedules, increased employee awareness and an aging workforce. Since the causes of these injuries in health care professionals are multifactorial, a variety of solutions are required to reduce worker risk.3
An ergonomically-designed workstation is only one of several solutions for minimizing worker injury in these departments. Training workers to improve their work postures and properly use the ergonomic features of their new & current equipment are also an important part of reducing injury risk. The impact of ergonomic considerations can result in increased productivity and quality of patient care, decreased number of lost workdays, fewer injuries and reduction in insurance costs.
Discussion
Occupational injuries are the main reason for longterm absence among ultrasound professionals.3,11 Each ultrasound specialty has unique tasks with injuries that are specific to those tasks. Technological advances have resulted in vascular labs becoming more efficient and productive, but they have added to the risk for worker injury. Vascular labs are adding more exams to their protocols, such as venous reflux exams and surveillance for temporal arteritis. Protocols for these exams do not include suggestions for scanning techniques and comfortable body postures. Epidemiologic and biomechanical studies have supported a causal relationship between workplace exposures and the occurrence of WRMSDs of the back and upper extremities. The severity of WRMSDs has been shown to be related to the performance of tasks that require forceful movements, with or without repetitive motion and static or awkward posture.2 The increasing use of technology has resulted in workers being able to accomplish the same work tasks with less movements. Thus, the relationship between the user and the workstation equipment has become “frozen,” and the worker is often forced into a static posture. These prolonged static postures result in musculoskeletal discomfort and eventually injury.
 Injury risk factors include forceful exertions, awkward postures and prolonged static postures, repetitive motions, “pinch” grip, and exposure to environmental factors such as extreme heat, cold, humidity or vibrations. The accumulated exposure to one or more of these risk factors over time leads to injury because repeated exposure interferes with the ability of the body to recover. WRMSDs cause pain, inflammation, swelling, deterioration of tendons and ligaments and spinal degeneration. Muscles and joints are further stressed once their support structures are weakened.
Injury risk factors include forceful exertions, awkward postures and prolonged static postures, repetitive motions, “pinch” grip, and exposure to environmental factors such as extreme heat, cold, humidity or vibrations. The accumulated exposure to one or more of these risk factors over time leads to injury because repeated exposure interferes with the ability of the body to recover. WRMSDs cause pain, inflammation, swelling, deterioration of tendons and ligaments and spinal degeneration. Muscles and joints are further stressed once their support structures are weakened.
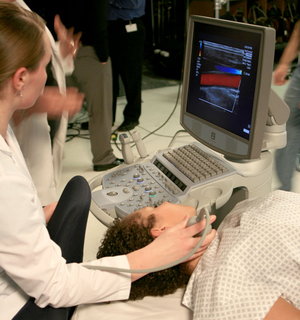
Among those performing vascular ultrasound exams, the upper extremities and the neck are the areas with the highest rate of injury.12 Those sonographers often scan with their arm unsupported and abducted more than 30 degrees from the body. They often have extended reaches to the patient and to the control panel of the ultrasound system. The farther one reaches, the shorter the endurance time for shoulder muscles. At a reach of 50 cm from the body, significant muscle fatigue will occur in less than 10 minutes.7 This ultimately sets the stage for muscle injury. The ideal reach should be no greater than 30 cm.
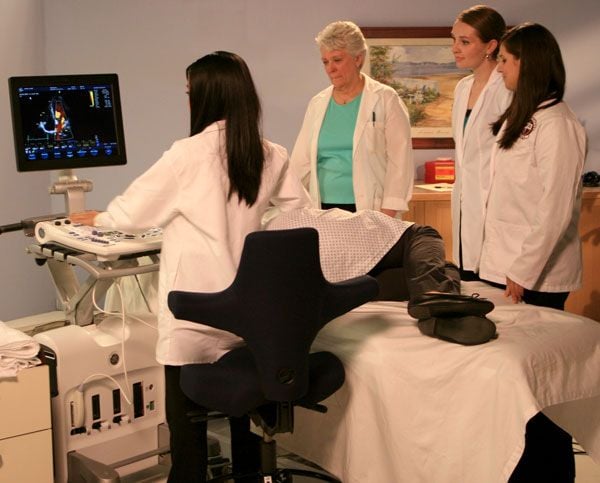
Neck pain is caused by inappropriate positioning of the ultrasound system monitor. Too often those performing exams fail to optimize the position of the ultrasound monitor, which forces them to twist the neck to view the image during the exam and other procedures associated with the exam. Oftentimes the ultrasound monitor is shared by the sonographer and the vascular surgeon during a procedure, which results in awkward neck postures when both are attempting to view the monitor.
Additionally, the increased use of computers in medical practices has changed the work tasks of health care professionals. Patient files are now reviewed at computer workstations and ultrasound images are viewed on PACS (picture archiving and communication system), resulting in prolonged periods of seated, static postures. The symptoms experienced are related to computer use and workstation design. Computer workstations are generally shared by a number of different practitioners during the day, which makes adjustability an important feature of workstation design.4
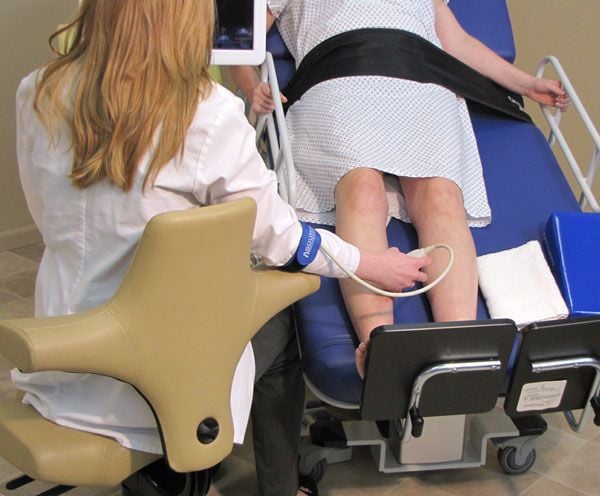
Sustained awkward postures can cause imbalances between the muscles that move and the muscles that stabilize. Repeatedly rotating the head, neck and trunk causes one set of muscles to become stronger and shorter and the opposing muscles to become weaker and elongated. Asymmetric forces are exerted on the spine causing misalignment. Nerve entrapment syndromes can result from increased muscle pressure on major nerves that run behind tightened muscles. Tasks that require the worker to continually lean forward, or bend the head down or laterally are examples of these types of postures.14
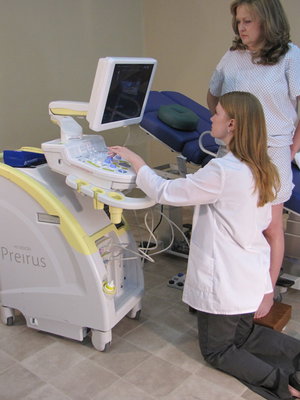
Prolonged static postures, whether sitting or standing, increase the load on soft tissues and the compressive forces on the spine. Additionally, the contraction of more than 50 percent of the body’s muscles is required to maintain static postures.14 Human physiology depends on movement which promotes normal muscle contraction and relaxation. Muscle activity circulates blood to carry nutrients to and remove toxins from muscles. Awkward and static postures cause muscles to continuously be contracted; therefore, they cannot receive oxygen or get rid of toxins.7 Since the onset of the Industrial Revolution and increasing computerization of the workplace, more jobs are becoming sedentary.5,14 The lack of movement necessary to perform many jobs has contributed to increased productivity, but it has also resulted in an increase in MSDs. Static postures require more than 50 percent of the body’s muscles to contract to hold the body motionless while resisting gravity.14 The intervertebral discs of the spine resist compression and shear forces, thus facilitating motion of the spine.10,13 However, excessive compressive forces and the decreased circulation that result from static postures cause microfractures. The strain on surrounding soft tissues increases, resulting in further injury. Vascular ultrasound exams and interventional procedures often result in static postures, as well as overreach and arm abduction.
Identifying and mitigating injury risks in the vascular lab begin with an on-site workstation assessment. Each industry & profession has very specific job requirements and work tasks. Ergonomics consultants and physical/occupational therapists can review and provide advice on general job tasks that are common to many industries– such as, good seated posture, proper set-up for a computer workstation, adequate lighting, etc.
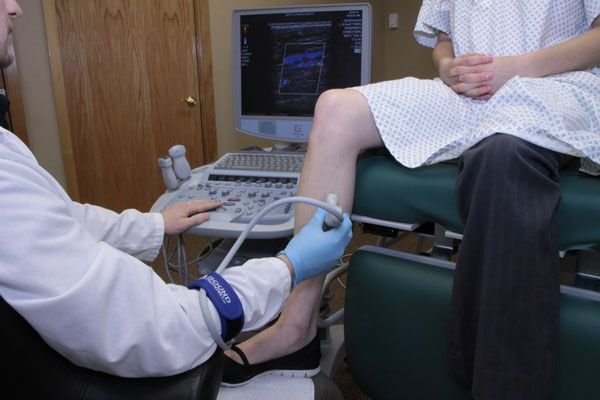
However, as with many professions, vascular ultrasound has very specific work tasks, and these are best evaluated by ergonomics consultants who are also industry experts. The assessment will identify at-risk work postures through the observation of workers performing various work tasks. The consultants can then make suggestions for postural changes that are practical and fit in with each individual’s work style. The exam room and computer workstation setups should be evaluated and suggestions for more functional and comfortable arrangement of the equipment can then be made. A detailed, illustrated report of findings and possible solutions should be provided for educational and reference purposes.
Conclusion
A study by Levanon, et al. demonstrated a significant reduction in WRMSD scores of the workers who participated in an intervention program.9 Identifying the appropriate ergonomic interventions for each worksite and for various work tasks should begin with an on-site assessment of the work environment. Ergonomics, the science of adapting the job to the employee, strives to prevent occupational musculoskeletal injuries by removing barriers to quality, productivity and human performance. Ergonomics can be utilized in health-care professions to increase efficiency, reduce errors, improve quality patient care, increase employee retention and satisfaction, and ultimately improve profits.
References
- Baker, N.A., Jacobs, K., Tickle-Degnen, L (2003). The association between the meaning of working and musculoskeletal discomfort. International Journal of Industrial Ergonomics, 31, 235-247.
- Barr, A.E., Safadi, F.F., Gorzelany, I., Amin, M., Popoff, S.N., Barbe, M.F. (2003). Repetitive, negligible force reaching in rates induces pathological overloading of upper extremity bones. Journal of Bone and Mineral Research, 18 (11), 2023-2032.
- Bongers, P.M., deWinter, C.R., Kompier, M.AJ., Hildebrandt, V.H. (1993). Psychosocial factors at work and musculoskeletal disease. Scandinavian Journal of Work Environment & Health, 19 (5), 297-312.
- Chesson, E. (2004). Creating the perfect soft-copy reading room. Health Imaging and IT, April, 48-52.
- Ergoweb, Inc. (2001). Applied Workplace Workplace Ergonomics Training Workbook, September 2001.
- Gabel, C.L., Gerberich, S.G. (2001). Risk factors for injury among veterinarians. Ergonomics, 13(1), 80-86.
- Kroemer, K., Grandjean, E. (2000). Fitting The Task to the Human, (5th ed.), Taylor & Francis, Inc., Philadelphia.
- Kumar, S., Moro, L., Narayan, Y. (2003). Morbidity among x-ray technologists. International Journal of Industrial Ergonomics, 33, 29-40.
- Levanon, Y., Fegen, A., Yehuda, L., Givon, U., Ratzon, N. (2012) Reducing musculoskeletal disorders among computer operators: comparison between ergonomics interventions at the workplace. Ergonomics, 55:12, 1571-1585.
- Luoma, K., Riihimaki, H., Raininki, R., Luukkonen, R., Lamminen, A., Viikari-Juntura, E. (1998). Lumbar disc degeneration in relation to occupation. Sandinavian Journal of Work, Environment, & Helath, 24(5), 358-366.
- Magnavita, N., Bevilacqua, L., Mirk, P., Fileni, A., Castellino, N., (1999). Work-related musculoskeletal complaints in sonologists. Journal of Occupational & Environmental Medicine, 41(11), 981-985.
- Pike, I., Russo, A., Berkowitz, J., et al (1997). The Prevalence of Musculoskeletal Disorders Among Diagnostic Medical Sonographers. Journal of Diagnostic Medical Sonography, 13(5), 219-227.
- Pope, M.H., Goh, K.L., Magnusson, M.L. (2002). Spine Ergonomics. Annual Review of Biomedical Engineering, 4, 49-68
- Valachi, B., Valachi, K. (2003). Mechanisms leading to musculoskeletal disorders in dentistry. Journal of the American Dentistry Association, October (134), 1344-1350.


