Fibrosis: An overlooked complication of venous disease impacting surgical success
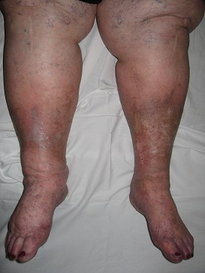 CHRONIC SWELLING is a common complication of venous disease, signifying both venous and lymphatic insufficiency, and is referred to as phlebolymphedema (Cavezzi, Lee). Soft tissue fibrosis is a common sequela of phlebolymphedema, with numerous etiologies, but common to all fibrosis is the potential to obstruct circulation, create pain, and limit movement and function (Földi 2012).
CHRONIC SWELLING is a common complication of venous disease, signifying both venous and lymphatic insufficiency, and is referred to as phlebolymphedema (Cavezzi, Lee). Soft tissue fibrosis is a common sequela of phlebolymphedema, with numerous etiologies, but common to all fibrosis is the potential to obstruct circulation, create pain, and limit movement and function (Földi 2012).
Vascular surgery effectively ameliorates symptoms in many patients, but patients with more complex recalcitrant swelling, such as those classified CEAP C3 and above, are likely to have more fibrosis to begin with. They are also more likely to have complications and persistent swelling following vascular surgery (Disselhoff, Földi 2000, Pittaluga).
Identifying common types of phlebolymphedema-related fibrosis
Lymphostatic fibrosis is a progressive inflammatory process in chronic edema, characterized by fibrosclerotic changes in tissue. It is formed by lymph stasis, which attracts fat cells that bind to surrounding tissues. Lymphostatic fibrosis first presents as soft, fatty tissue—it can be mistaken for swelling—but it does not reduce and becomes harder and larger over time as superficial cutaneous lymphatics become obliterated (Butcher).
In extreme and advanced cases of phlebolymphedema, especially those compounded by obesity, hard, overhanging lobules can form along the ankle and leg that interfere with mobility. Lymphostatic fibrosis is present in all patients with chronic swelling with varying degrees of severity, even those classified as lymphedema stage 0 without detectible edema (Földi 2012). Thus, some patients with CEAP classification C0 may have latent edema and, therefore, sclerotic changes, even before progressing to identifiable edema: CEAP stage C3.
Stemmer’s sign (also called Kaposi-Stemmer’s sign) is a clinical test for lymphedema. It is positive when the skin on the top of the second toe (or index finger) is thickened and the skin cannot lift when it is pinched. This occurs in toes with profuse swelling and also with toes that have developed lymphostatic fibrosis (Brenner).
Lipodermatosclerosis (LDS) is a painful inflammatory process in which a constrictive panniculitis is formed in the dermis surrounding the ankle and lower leg. This band of hard, fibrotic tissue gives lower legs the characteristic inverted champagne bottle or bowling pin shape, with small ankles and large, swollen calves. It is usually bilateral and can mimic cellulitis in the early stages (Farrow, Mortimer 2018).
Post-thrombotic syndrome is a frequent complication of deep vein thrombosis (DVT) that can create a myriad of symptoms, including thickened tissues, which obstruct venous and lymphatic circulation (Bouman, Kahn). In addition to anticoagulation, compression treatment post-thrombosis is recommended to resolve symptoms and prevent reoccurrence (Chibbaro).
Scar tissue from surgery or trauma can create stasis by mechanical obstruction to venous and lymphatic circulation (Fernandez, Földi 2012) and can worsen chronic lymphedema (Lynch). Scar tissue is associated with impairment in lymphatic regeneration (Avraham) and can trap lymphedema (Warren).
Post-cellulitis fibrosis can occur with venous and lymphatic insufficiency. Those with lymphedema have a 71-fold risk over the normal population (Dupuy, Mortimer 2014). The damaged post-cellulitis tissues can become hyperkeratotic, and lymphatic pathways can be obliterated (de Godoy). The resultant impaired local circulation makes infectious reoccurrence more likely (Al-Niaimi, de Godoy, Tay).
Wound-related fibrosis
Scarring is common following closure of large or deep wounds, and poor vascular and lymphatic circulation impacts the rate of healing and quality of the scar (Cedidi, Marshall, Singer, Son). Chronic, nonhealing venous leg ulcers (VLU) can display a “bed” of dense, fibrotic tissue surrounding the wound as well as plaques of biofilm in the wound bed that inhibit local circulation and wound closure (Malone, Raghow).
Atrophie blanche, also known as livedo vasculitis, is identifiable by star-shaped or polyangular hypopigmented scarring due to alterations in microcirculation in which capillaries are decreased and even absent. These damaged areas are prone to repeated ulceration and further scarring (Amital, Maessen-Visch).
Dermal fibrosis results from chronic inflammation associated with severe phlebolymphedema. It is often a byproduct of stasis and ulceration with debilitated lymphatic circulation to the dermis (Fernandez).
Forms of dermal fibrosis
Hyperkeratosis is caused by an overproduction of keratin, producing nodules on the surface of the skin. These can vary in size from small, “mossy” patches (papillomatosis) to raised, wart-like growths (papillomas). These nodules are often pruritic and can be worsened when patients scratch them. In rare cases with long-standing lymphedema, malignant tumors develop (lymphangiosarcomas). Topical medication can be of some use, but underlying swelling must be addressed (Fife, Földi 2012, Gianesini 2018).
Stasis dermatitis is a direct consequence of venous hypertension and creates hypoxia and cell death from the disruption of microcirculation and the creation of fibrin cuffs (Farrow). It is characterized by hemosiderin deposits, eczematous, and atrophic dermal patches with the medial ankle most commonly affected.
Proximal fibrosis that is not directly related to venous disease can significantly influence circulation in the feet and legs and contribute to the progression of phlebolymphedema. Damage to structures in the abdomen, trunk, genitals, and proximal legs by means such as surgery, trauma, or radiation therapy can negatively impact lower extremity circulation by interrupting proximal lymphatic circulation. Common etiologies include treatment for reproductive cancers, inguinal lymph node dissection for lower extremity melanoma, and even total hip replacement surgery.
Treatment for fibrosis
Treatment for fibrosis has two phases: first addressing swelling, and then treating fibrotic obstruction.
Phase I: Treating swelling
Decongestion evacuates swelling from the feet and legs, and it is essential to immediately apply compression to preserve results and prevent reflux. Manual lymphatic drainage (MLD) is the gold standard of treatment both for the reduction and maintenance of swelling (Földi 2012, Molski).
Intermittent pneumatic compression (IPC) is both a decongestive and compressive treatment proven to be a more effective in-home treatment than MLD (Wilburn). This is particularly true for patients with limitations in strength, range of motion, and endurance. IPC treats phlebolymphema using a mechanized gradient sequential compression system and is known to accelerate wound healing and prevent cellulitis infections (Brayton, Comerota, Lantis). IPC equipment is covered by many insurances, including Medicare, with requirements of a qualifying diagnosis and persistent swelling despite a home trial of elevation, exercise, and compression garments (Centers for Medicare and Medicaid Services).
Elevation harnesses the effects of gravity to facilitate lymphatic and venous return. Leg positioning is an important consideration for those who are sedentary with impaired mobility. Particularly vulnerable are those who spend waking and sleeping hours in a reclining chair with legs in a dependent or semi-dependent position. Many of these so-called “armchair patients” seek an upright torso position of comfort to ameliorate comorbidities such as asthma, back pain, or obstructive sleep apnea (Stignant). Patients with mixed disease may find elevating legs to be painful due to decreased arterial circulation (Martin-Du Pan). These issues need to be addressed in order to allow better positioning options to facilitate improved venous and lymphatic return (Cook) and to ultimately ameliorate phlebolymphema and arrest the progression of lymphostatic fibrosis.
Compression garments and bandaging provide external pressure against veins and lymphatics to compensate for valvular incompetence and reflux by improving hemodynamics and the effectiveness of the calf muscle pump (Ibegbuna, Mortimer 2004, O’Brien). The use of compression is well-documented post venous surgery (Bakker, Biswas, Chou, Elderman, Lurie [2019], Nootheti, Onwudike, Reich-Schupke, Wittens, Ye). Chronic edema requires continuous compression (Moffatt 2012). Gradient elastic stockings are generally used for maintenance and for milder swelling. Layered short-stretch bandages or Velcro compression wraps are used for initial reduction and ongoing treatment of very swollen feet and legs, and disposable compression wraps are a component of wound care (International Society of Lymphology Executive Committee, Wittens).
Skincare is essential for the treatment and prevention of wounds. Feet and legs should be cleaned and dried daily, and fungal infections should be addressed promptly. Xerosis and frail skin increase wound risk factors and require conditioning with emollients. Topical medications may be indicated, but bacitracin and neomycin should be avoided because they are frequent allergens and can provoke contact dermatitis (Farrow, Fife, Herrick, Holloway).
Exercise, particularly ankle movement in walking, is a critical factor in venous and lymphatic circulation (Lattimer, Padberg, Strobenreuther). The veins and lymphatics rely on muscle pump action of the calf muscles for upward circulation against gravity. There is a correlation between the “shuffle gait” and limited ankle range of motion producing reduced calf muscle contraction, yielding impaired circulation (Kan). This deterioration in function correlates with the development of CVI (chronic venous insufficiency) and venous ulcers (Back). Those with paresis or paralysis of the lower legs are particularly vulnerable to swelling. Diaphragmatic breathing has been shown to improve lower leg venous circulation (Aliverti, Miller, Willeput).
For those with intact and healthy skin, aquatic exercise gives an added benefit of gradient water compression and has been shown to increase ankle flexibility and decrease chronic leg edema (Gianesini 2016). Stevin’s law demonstrates that the deeper the water, the greater the water compression. For example, exercising at a depth of one meter yields 74 mmHg of pressure on the feet (Wilcock).
Education empowers patients to reduce risk factors for swelling and infection. Lifestyle changes may be indicated, including smoking cessation, weight loss, increasing activity, and mobility, and adherence to a home swelling management program (Labropoulos).
Lifestyle changes may be indicated, including smoking cessation, weight loss, increasing activity, and mobility, and adherence to a home swelling management program.”
Phase 2: Treating fibrotic obstructions
Many of the above-mentioned treatments for swelling also help fibrosis. Increased pressure is required to remodel areas of heavy fibrotic damage and to effectively move swelling trapped inside and underneath the fibrotic tissue (Földi 2012). It is important to adjust treatment if there is fragile skin or paresthesia.
Compression bandaging and garments can facilitate both circulation and fibrosis remodeling and utilize textured, irregular surfaces to mechanically soften the dermis and deeper tissues. Typical examples are channeled foam, chipped form pieces quilted into pads or garments, and elastic garments with a textured weave.
The negative spaces in the surface of the garment direct fluid out of swollen areas and create a micro-massage to soften hardened areas (Farrow, Zuther). Increasing external compression and bulk can increase effectiveness, but additional bulk may impede joint motion and make it more difficult to walk, making it less of an ongoing day- time treatment and a more popular nocturnal choice.
Manual therapy and instrument-assisted techniques utilize specialized massage and tools to create a controlled microtrauma to remodel fibrotic tissue (Baker, Chughtai). Various tools can be used to produce deep massage, negative pressure, and vibration. The use of a low-level 904 nm nonthermal laser in conjunction with these techniques can enhance this process by addressing fibrosis and ameliorating inflammation (Fillipin).
Skincare may need to be upgraded with topical medications to address specific types of dermal fibrosis (Fife).
IPC used at higher pressures (>50 mmHg) remodels fibrotic tissues and creates new deep lymphatic channels when superficial lymphatics are obliterated by fibrosis (Olszewski, Zaleska). The amount of pressure should be titrated to ensure the treatment is both effective and comfortable. Patients with wounds or diabetic neuropathy may tolerate higher pressures with the use of specific IPC devices that have features such as wave-like programming, rapid inflation, faster cycle time, and long pause timers between compression cycles to increase comfort and lymphatic uptake during high-compression treatment.
Faster cycle time has been proven to be superior in healing VLU (Nikolovska). Anti-fibrotic compression garments or pads, as described above, can be used concurrently with pneumatic compression to enhance remodeling effects.
Conclusion
Fibrosis is a less frequently identified component of chronic venous disease that is known to compound circulatory impairment. Addressing swelling and fibrosis conservatively should be considered prior to perform venous procedures with complex patients, both to manage swelling prior to surgery and as aftercare.
Bibliography
Al-Niaimi F, Cox N (2009) Cellulitis and lymphoedema: a vicious cycle. Journal of Lymphoedema 4(2):38-42.
Aliverti A et al (2009) The abdominal circulatory pump PLoS ONE 4(5): e5550. Doi:10.1371/journal.pone.0005550
Amital H et al (2000) Use of intravenous immunoglobulin in livedo vasculitis. Clinic and Experimental Rheumatology 18: 404-406.
Avraham T et al (2009) Fibrosis Is a Key Inhibitor of Lymphatic Regeneration. Plastic and Reconstructive Surgery 124(2): 438-350.
Back T et al (1995) Limited range of motion is a significant factor in venous ulceration. Journal of Vascular Surgery 22: 519-523.
Baker R et al (2013) Instrument-assisted soft tissue mobilization treatment for tissue extensibility dysfunction. International Journal of Athletic Therapy & Training 18(5): 16-21.
Bakker N A (2013) Compression stockings after endovenous laser ablation of the great saphenous vein: a prospective randomized controlled trial. European Journal of Vascular and Endovascular Surgery 46(5): 588-592.
Biswas S et al (2007) Randomised clinical trial of the duration of compression therapy after varicose vein surgery. European Journal of Vascular and Endovascular Surgery 33:631-637.
Bouman A C (2016) Post-thrombotic syndrome, exploring aspects of pathophysiology and personalized management. Promovendi CD, RS: CARIM - R1 - Thrombosis and haemostasis, RS: CAPHRI - R2 - Creating Value-Based Health Care, Interne Geneeskunde. Accessed July 2020 https://cris.maastrichtuniversity.nl/en/publications/post-thrombotic-syndrome-exploring-aspects-of-pathophysiology- https://www.narcis.nl/publication/RecordID/oai:cris.maastrichtuniversity.nl:publications%2F340f36f0-6984-43ae-b0b0-5fc6bfc22bbf
Brayton K et al (2014) Lymphedema prevalence and treatment benefits in cancer: impact of a therapeutic intervention on health outcomes and costs. PLoS ONE 9(12): e114597 doi:10.1371/journal.pone.0114597
Brenner E et al (2007) Stemmer’s (Kaposi-Stemmer-) sign – 30 years later. Phlebologie 36: 320-324.
Butcher H, Hoover A (1955) Abnormalities of human superficial cutaneous lymphatics associated with stasis ulcers, lymphedema, scars and cutaneous autografts. Annals of Surgery 142(4): 633-653.
Cavezzi A (2018) Diagnosis and management of secondary phlebolymphedema. In: BB Lee, S Rockson, J Bergan (Eds.) Lymphedema: A concise compendium of theory and practice (pp. 925-953). 2nd ed. Switzerland: Springer.
Cedidi C C, Ingianni G (2006) Compression therapy after complex soft tissue trauma, and flap coverage: optimization of scar development, swelling, function, and aesthetic result. European Journal of Medical Research 11: 85-89.
Centers for Medicare and Medicaid Services (2002) National coverage determination for pneumatic compression devices publication 100-3. Accessed from cms.gov July 2020.
Chibbaro S et al (2018) Evolution of Prophylaxis Protocols for Venous Thromboembolism in Neurosurgery: Results from a Prospective Comparative Study on Low-Molecular-Weight Heparin, Elastic Stockings, and Intermittent Pneumatic Compression Devices. World Neurosurgery 109: e510-516.
Comerota A (2011) Intermittent pneumatic compression: physiologic and clinical basis to improve management of venous leg ulcers. Journal of Vascular Surgery 53(4): 1121-1129.
Chou J-H et al (2019) Optimal duration of compression stocking therapy following endovenous thermal ablation for great saphenous vein insufficiency: a meta-analysis. International Journal of Surgery 65:113-119.
Chughtai M et al (2019) Astym® therapy: a systematic review. Annals of Translational Medicine 7(4):70. Doi:10.21037/atm.2018.11.49
Cook L (2012) Challenges to effective treatment of lower-limb oedema. British Journal of Community Nursing 17(Sup4): S4-S10.
deGodoy J M P et al (2000) Lymphoscintigraphic evaluation in patients after erysipelas. Lymphology 33: 177-180.
Disselhoff BCVM et al (2008) Is there a risk for lymphatic complications after endovenous laser treatment versus Phlebology 23:10-14.
Dupuy A et al (1999) Risk factors for erysipelas of the leg (cellulitis): case-control study. BMJ 318(2198): 1591-1594.
Elderman J et al (2014) Role of compression stockings after endovenous laser therapy for primary wounds. Journal of Vascular Surgery: Venous and Lymphatic Disease 4(2): 289-296.
Farrow W (2010) Phlebolymphedema- a common underdiagnosed and undertreated problem in the wound care clinic. The Journal of the American College of Certified Wound Specialists 2(1): 14-23.
Fernandez A et al (2011) Histopathologic analysis of dermal lymphatic alterations in chronic venous insufficiency ulcers using D2-40. J Am Acad Dermatol 64; 1123.e1-12.
Fife C E et al (2017) Skin and wound care in lymphedema patients: a taxonomy, primer and literature review. Advances in Skin and Wound Care 30(7): 305-318.
Fillipin L I et al (2004) Low‐level laser therapy (LLLT) prevents oxidative stress and reduces fibrosis in rat traumatized Achilles tendon Lasers Surg Med. 37(4): 293-300.
Földi M, Idiazabal G (2000) The role of operative management of varicose veins in patients with lymphedema and/or lipedema of the legs. Lymphology 33:167-171.
Földi M (2012) Chronic venous insufficiency (CVI.) In: M Földi, E Földi, S Kubik, (Eds.) Textbook of Lymphology for Physicians and Lymphedema Therapists (pp. 373-386) 3rd ed. Munich: Urban & Fischer.
Földi M, Földi E (2012) Treatment of lymphostatic fibrosis. In: M Földi, E Földi, S Kubik, (Eds.) Textbook of Lymphology for Physicians and Lymphedema Therapists (p. 484). 3rd ed. Munich: Urban & Fischer.
Gianesini S et al (2018) Management of phlebolymphedema ulcer. In: BB Lee, S Rockson, J Bergan (Eds.) Lymphedema: A concise compendium of theory and practice (pp. 937-953). 2nd ed. Switzerland: Springer.
Gianesini S et al (2016) A specifically designed aquatic exercise protocol to reduce chronic lower limb edema. Phlebology 32(9): 594-600.
Gloviczki P, Lawrence P (2020) Venous and lymphatic disorders excels in quality, impact, and teamwork. Journal of Vascular Surgery 8(1): 1-7.
Herrick S et al (2002) Dermal changes in the lower leg skin of patients with venous hypertension. International Journal of Lower Extremity Wounds 1(2): 80-86.
Holloway S (2019) Skin considerations for older adults with wounds. Community Wound Care 24(Supp 6): S15-S19. https://doi.org/10.12968/bjcn.2019.24.Sup6.S15
Ibegbuna V, Delis K (2003) Effect of compression stockings on venous hemoynamics during walking. Journal of Vascular Surgery 37: 420-425.
International Lymphoedema Framework (2012) Best practice for the management of lymphoedema. 2nd ed. Compression therapy: a position document on compression bandaging. Accessed from www.lympho.org.
International Society of Lymphology Executive Committee (2020) The diagnosis and treatment of peripheral lymphedema: 2020 consensus document of the international society of lymphology. Lymphology 53(1): 3-19.
Kahn S et al (2016) Guidance for the prevention and treatment of the post-thrombotic syndrome. J Thromb Thrombolysis 41:144-153.
Kan Y M, Delis K T (2001) Hemodynamic effects of supervised calf muscle exercise in patients with venous leg ulceration. Arch Surg 1364-1369.
Labropoulis N (2019) How does chronic venous disease progress from the first symptoms to the advanced stages? A review. Adv Ther 36: S13-S19. https://doi.org/10.1007/s12325-019-0885-3
Lantis J et al (2011) The effect of percutaneous intervention on wound healing in patients with mixed arterial-venous disease. Ann Vasc Surg 25(1): 79-86.
Lattimer C et al (2017) Optimizing calf muscle pump function. Phlebology 33, 353-360. DOI: 10.1177/0268355517709410
Lee, B B (2020) Phlebolymphedema: neglected outcome of combined venous and lymphatic insufficiency. Vascular Specialist International 36(1):1-3. https://doi.org/10.5758/vsi.2020.36.1.1
Lurie F et al (2020) CEAP classification system and reporting standard, revision 2020. Journal of Vascular Surgery: Venous and Lymphatic Disorders article in press https://doi.org/10.1016/j.jvsv.2019.12.075
Lurie F, De Maseseneer, M (2020) The 2020 update of the CEAP classification: what is new? European Journal of Endovascular Surgery 59, 859-860.
Lurie F et al (2019) Compression therapy after invasive treatment of superficial veins of the lower extremities: Clinical practice guidelines of the American Venous Forum, Society for Vascular Surgery, American College of Phlebology, Society for Vascular Medicine, and International Union of Phlebology Society for Vascular Surgery Document 7(1): P17-28. doi:https://doi.org/10.1016/j.jvsv.2018.10.002
Lynch L et al (2015) Fibrosis worsens chronic lymphedema in rodent tissues. Am J Physiol Heart Circ Physiol 308: H1229-H1236.
Lv S et al (2017) A review of the postoperative lymphatic leakage. Oncotarget 8(40): 69062-69075.
Maessen-Visch M B (1999) Atrophe blanche. International Journal of Dermatology 38:161-172.
Malone M et al (2017) The prevalence of biofilms in chronic wounds: a systemic review and meta-analysis of published data. Journal of Wound Care 26(1): 20-25.
Marshall C et al (2018) Cutaneous scarring: basic science, current treatments and future directions. Advances in Wound Care 7(2): 29-44.
Martin-Du Pan R et al (2004) The role of body position and gravity in the symptoms and treatment of various medical diseases. Swiss Med Wkly 134: 543-551.
Miller J et al (2005) Skeletal muscle pump versus respiratory muscle pump: modulation of venous return from the locomotor limb in humans. Journal of Physiology 563(3): 925-943.
Moffat C et al (2012) Compression therapy: a position document on compression bandaging. International Lymphoedema Framework Best practice for the management of lymphoedema, 2nd edition. accessed July 2020 www.lympho.org
Molski P et al (2009) Patients with venous disease benefit from manual lymphatic drainage. International Angiology 28(2): 151-156.
Mortimer P (2018) Cutaneous manifestations of edema. In: BB Lee, S Rockson, J Bergan (Eds.) Lymphedema: A concise compendium of theory and practice (pp. 205-219). 2nd ed. Switzerland: Springer.
Mortimer P, Rockson S (2014) New developments in clinical aspects of lymphatic disease. The Journal of Clinical Investigation 124(3)P 915-921.
Mortimer P, Levick J R (2004) Chronic peripheral oedema: the critical role of the lymphatic system. Clin Med 4: 448-453.
Nikolovska S et al (2005) Evaluation of two different intermittent pneumatic compression cycle setting in the healing of venous ulcers: a randomized trial. Med Sci Monit 11(7): CR337-343.
Nootheti P et al (2008) Efficacy of graduated compression stockings for an additional 3 weeks after sclerotherapy treatment of reticular and telangietctatic leg veins. Dermatological Surgery 35:53.58. doi: 10.111/j.1524-4725.2008.34382.x
O’Brien J A et al (2012) Understanding the relationships between the calf muscle pump, ankle range of motion and healing venous leg ulcers: a review of the literature. Wound Practice & Research 20(2): 80-85.
Olszewski WL et al (2011) Pathways of lymph and tissue fluid flow during intermittent pneumatic massage of lower limbs with obstructive lymphedema. Lymphology 44(2):54-64.
Onwudike M et al (2020) Role of compression after radiofrequency ablation of varicose veins: a randomised controlled trial. European Journal of Vascular and Endovascular Surgery 60: 108-117.
Padberg F et al (2003) Structure exercise improves calf muscle function in chronic venous insufficiency: a randomized trial. Journal of Vascular Surgery 39: 79-87.
Pittaluga P, Chastanet S (2012) Lymphatic complications after varicose veins surgery: risk factors and how to avoid them. Phlebology 27 Suppl 1: 139-142.
Raghow R (1994) The role of extracellular matrix in postinflammatory wound healing and fibrosis. The FASEB Journal 8: 823-831.
Reich-Schupke S (2014) Efficacy and comfort of medical compression stockings with low and moderate pressure six weeks after vein surgery. Phlebology 29:358-366.
Singer A, Clark R (1999) Cutaneous wound healing. The New England Journal of Medicine 341; 738-746.
Son D, Harijan A (2014) Overview of surgical scar prevention and management. Journal of Korean Medical Science 29: 751-757.
Stignant A (2013)Tackling obesity as part of a lymphoedema management programme British Journal of Lymphoedema 14(Supp 5) doi.org/10.12968/bjcn.2009.14.Sup5.44504
Strobenreuther R H K et al (2012) Decongestive movement therapy, decongestive breathing therapy, rehabilitation exercise and other physical therapy techniques In: Földi M, Földi E, Kubik S, eds. Textbook of Lymphology for Physicians and Lymphedema Therapists. 3rd ed. Munich: Urban & Fischer.
Tay E et al (2014) Cellulitis recurrence score: a tool for predicting recurrence of lower limb cellulitis. J Am Acad Dermatol 72(1): 140-145.
Warren A, Slavin S (2007) Scar Lymphedema: Fact or Fiction? Ann Plast Surg 59(1): 41-45.
Wilburn O et al (2006) BMC Cancer 6:84 doi:10.1186/1471-2407-6-84
Wilcock I et al (2006) Physiological response to water immersion: a method for sport recovery. Sports Medicine 36(9): 747-765.
Willeput R et al (1984) Breathing affects venous return from legs in humans. J Appl. Physiol 57: 971-976.
Wittens C et al (2015) Clinical practice guidelines of the European society for vascular surgery. European Journal of Vascular and Endovascular Surgery 49:678-737
Ye K, et al (2016) Post-operative benefit of compression therapy after endovenous laser ablation for uncomplicated varicose veins: a randomized clinical trial. European Journal of Vascular and Endovascular Surgery. 52, 847-853.
Zaleska M et al (2015) Intermittent pneumatic compression enhances formation of edema tissue fluid channels in lymphedema of lower limbs. Lymphatic Research and Biology 13(2): 146-153.
Zuther J (2018) Application of compression bandages In: Zuther J & Norton S (Eds.) Lymphedema Management: The Comprehensive Guide for Practitioners 4th ed (397-416). Stuttgart: Georg Thieme Verlag.


